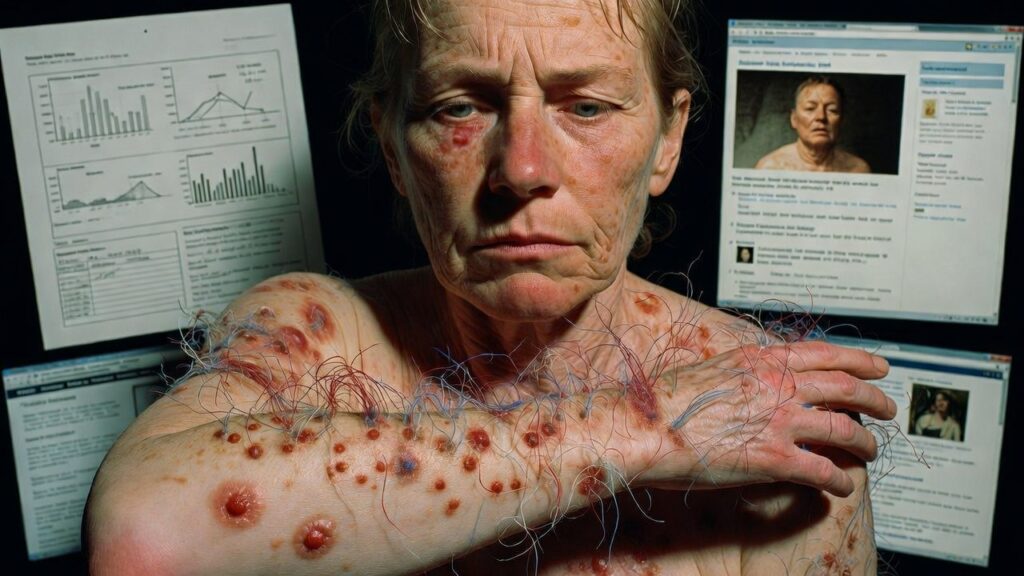
Picture this: You wake up in the dead of night, convinced that something is moving just beneath your skin. The sensation is relentless—crawling, biting, stinging—like invisible insects burrowing deeper with every passing second. You scratch until your skin breaks open, forming slow-healing sores that refuse to close. Then, from these wounds, strange fibers emerge: thin, colorful threads in shades of black, white, red, blue, or even metallic hues. You collect them, photograph them, show them to doctors—yet most are met with skepticism, a psychiatric label, or outright dismissal. This is the daily torment faced by people with Morgellons disease, a condition that has shattered lives while dividing the medical world.
For many sufferers, the ordeal begins subtly. It might start with an unexplained itch or a prickling feeling on the arms, legs, or scalp. Over weeks or months, the sensations intensify, spreading across the body. Lesions appear—often self-inflicted from desperate scratching—and the fibers become visible, sometimes moving or changing color under light. Accompanying these skin horrors are profound systemic effects: crushing fatigue that leaves you bedridden, joint pain mimicking arthritis, brain fog that clouds thinking, sleep disturbances, and emotional despair. Quality of life plummets dramatically; a 2025 study in the British Journal of Dermatology revealed that patients with Morgellons report worse impacts than those with severe psoriasis, atopic dermatitis, or prurigo nodularis—conditions already notorious for their burden.
One patient, after more than 15 years of battling the condition, described it as a life-altering invasion: sensations of ants crawling head to toe, followed by explosive lesions and protruding fibers in vivid, unnatural colors. Another recounted how the disease flares during immune crashes, linking it to chronic conditions like Lyme disease. These aren’t rare anecdotes; thousands share similar stories through support networks, forums, and advocacy groups. The isolation is crushing—families fracture, careers end, and hope fades when medical professionals insist the fibers are imaginary or environmental contaminants like cotton threads.
The name “Morgellons” itself carries historical weight. It harks back to a 17th-century description by Sir Thomas Browne of children afflicted with “harsh hairs” erupting from their backs. But the modern resurgence exploded in the early 2000s, sparked by biologist Mary Leitao, who observed bizarre blue and red filaments in her son’s non-healing lesions. She founded the Morgellons Research Foundation, and soon over 10,000 families registered similar experiences. What began as a grassroots movement has grown into a global phenomenon, fueled by online communities and documentaries that challenge the dominant narrative.
Imagine waking up every day feeling like insects are crawling beneath your skin, only to discover strange, colorful fibers emerging from slow-healing sores. For thousands of people worldwide, this isn’t a nightmare—it’s their reality. Morgellons disease, a condition shrouded in controversy and dismissal, has left sufferers isolated, desperate, and often labeled as delusional. But as new research emerges in 2026, the tide may be turning. This article dives into the evidence suggesting Morgellons is far more than a psychiatric illusion—it’s a complex, multisystem disorder demanding urgent attention.
The Harrowing Symptoms and Patient Experiences
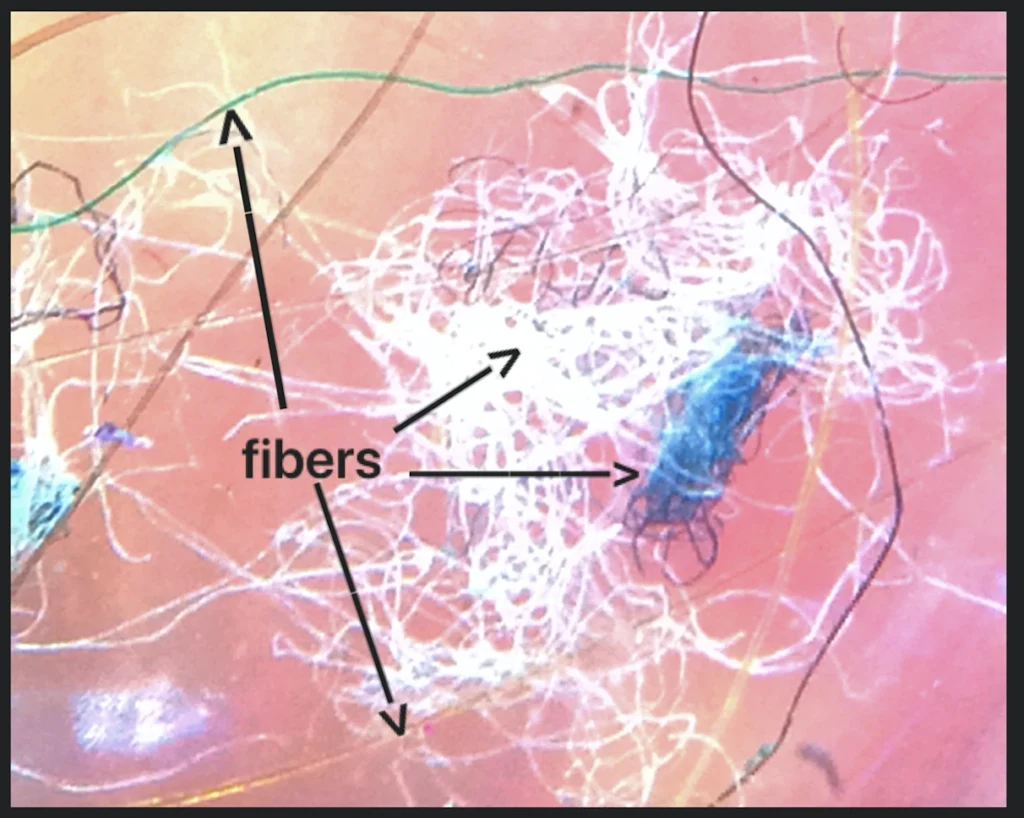
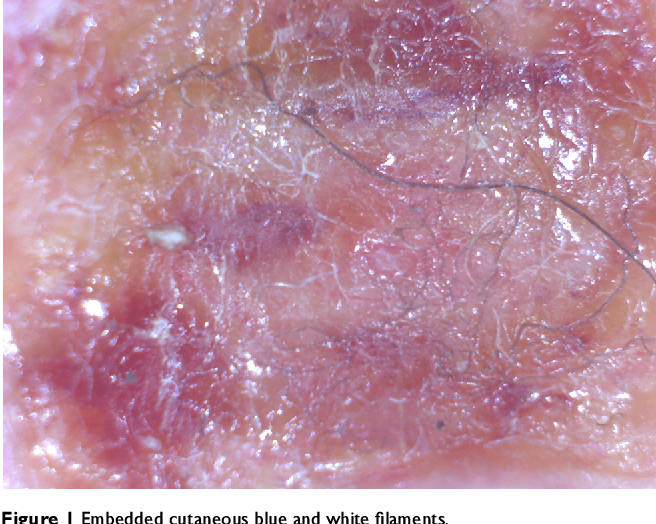
Morgellons disease typically presents with intense, unrelenting skin sensations: crawling, biting, stinging, or burning that drives victims to scratch relentlessly. Open lesions form, refusing to heal, and from them protrude bizarre fibers—often described as black, white, red, blue, or multicolored threads that seem to move on their own. Accompanying these are systemic issues like chronic fatigue, joint pain, cognitive fog, and even neurological symptoms.
Take the story of one long-time sufferer who shared on X: “I’ve had Morgellons Disease (MD) 27 years now. My last 5 years were as bad as My first two… It reproduces in your joints (all joints) then spread over you outer body.” This individual, who claims to have documented the disease’s progression with photos and videos, offers themselves for study, highlighting the parasitic-like nature of the condition. Another poster recounted battling it multiple times alongside diagnoses like Chronic Fatigue Syndrome and Fibromyalgia, noting it flares when the immune system crashes.
These aren’t isolated tales. A 2025 study published in the British Journal of Dermatology found that patients with Morgellons report a lower quality of life than those with psoriasis, atopic dermatitis, or prurigo nodularis—conditions already known for their debilitating impact. The distress is real, measurable, and profound.
To visualize the enigma, consider these microscopic views of the fibers and lesions reported by patients:
A History of Dismissal and the Mainstream View
The term “Morgellons” traces back to a 17th-century description, but the modern phenomenon exploded in the early 2000s via online communities. The pivotal 2012 CDC study examined 115 cases and concluded no infectious cause; the fibers were mostly cotton or skin proteins, and lesions stemmed from scratching. This led to its classification as delusional infestation, a psychiatric disorder where individuals falsely believe they’re infested despite evidence to the contrary.
Critics argue this label stigmatizes patients, complicating care. A recent Undark article from February 2026 highlights how language around Morgellons—like calling it “delusional”—hinders treatment, with dermatologists like Jesse Keller at Oregon Health and Science University advocating for destigmatization. Patients feel dismissed, echoing broader issues in medicine where women’s pain or unexplained symptoms are often psychologized.
Emerging Evidence: An Infectious Link?
Yet, a growing body of research challenges the purely psychiatric narrative. The Charles E. Holman Foundation, dedicated to Morgellons, reports ongoing studies linking it to persistent Borrelia infections—the bacteria behind Lyme disease. A 2023 Oklahoma State University study analyzed epithelial samples and suggested a tick-borne etiology, with spirochetes found in lesions. At the 2025 ILADS conference, new findings presented by OSU researchers reinforced this connection.
A 2025 JAAD International article notes public perception fueled by media like the 2019 documentary “Skin Deep,” which critiques the neuropsychiatric label and supports the Borrelia hypothesis. Even a 2025 case report in JAAD Case Reports described trigeminal trophic syndrome mimicking Morgellons, but treatment with nerve blocks succeeded only after addressing the underlying issue—hinting at neurological-infectious overlaps.
Podcasts and forums in 2026, like “More Morgellons,” discuss Clifford Carnicom’s work on environmental factors and potential bioengineering, though these remain speculative. A ResearchGate publication from late 2025 analyzes Morgellons as a multisystem problem, incorporating AI to explore hypotheses, and calls for unified diagnostic approaches.
X discussions often tie it to Lyme, with one user stating: “Morgellons and chronic Lyme disease are often connected, yet frequently treated as separate conditions.” Sufferers report flares after immune crashes, mirroring chronic infections.
Other strong book options:
- “Day One: A Morgellons Complete Guide for Newly Infected” (2025 beginner survival guide).
- “Morgellons Disease: Understanding the Symptoms, Causes, and Treatment” (enigmatic condition overview).
Treatment Challenges and Hope on the Horizon
Mainstream treatment focuses on antipsychotics like risperidone to alleviate delusions, combined with therapy and wound care. But those advocating an infectious model push antibiotics, with mixed results. A 2025 Instagram post emphasizes integrated care for Lyme-Morgellons overlaps.
The divide persists, but 2026 brings calls for compassion. As one X user put it, echoing broader medical gaslighting: “The 4 year trauma ended in a month” after proper diagnosis— a reminder that dismissal prolongs suffering.
Why We Must Take Morgellons Seriously
Morgellons isn’t a delusion for those living it—it’s a life-altering ordeal backed by mounting evidence of infectious roots. While the CDC’s stance holds sway, independent research and patient voices demand reevaluation. Dismissing it as “all in the head” ignores the fibers under microscopes, the Borrelia detections, and the ruined lives. In 2026, with AI aiding analysis and conferences spotlighting findings, it’s time for medicine to listen. If you’re suffering, seek specialists in Lyme or integrative dermatology—your pain is valid, and answers may be closer than ever.
Morgellon Art
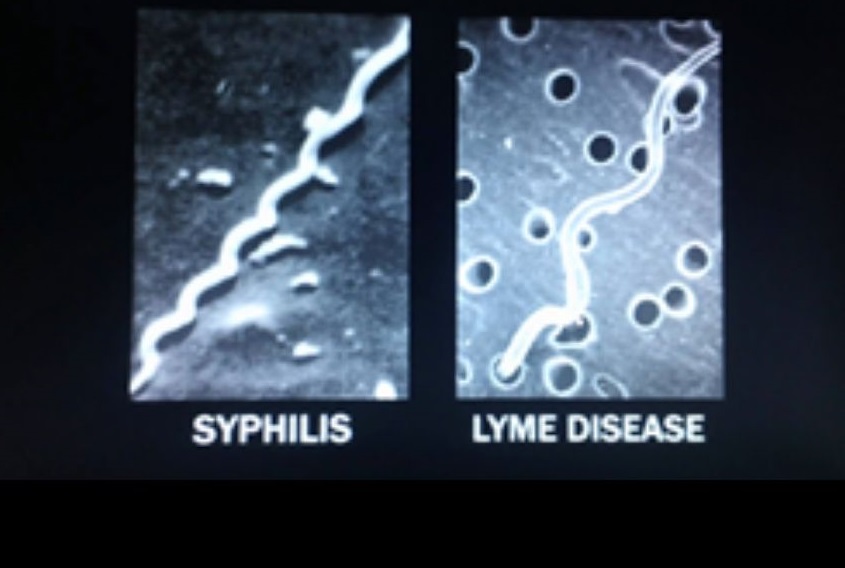





 Professor And Her Students May Have Found A Cure For Lyme Disease
Professor And Her Students May Have Found A Cure For Lyme Disease